I have another foot ulcer. Same Place. Same reason.
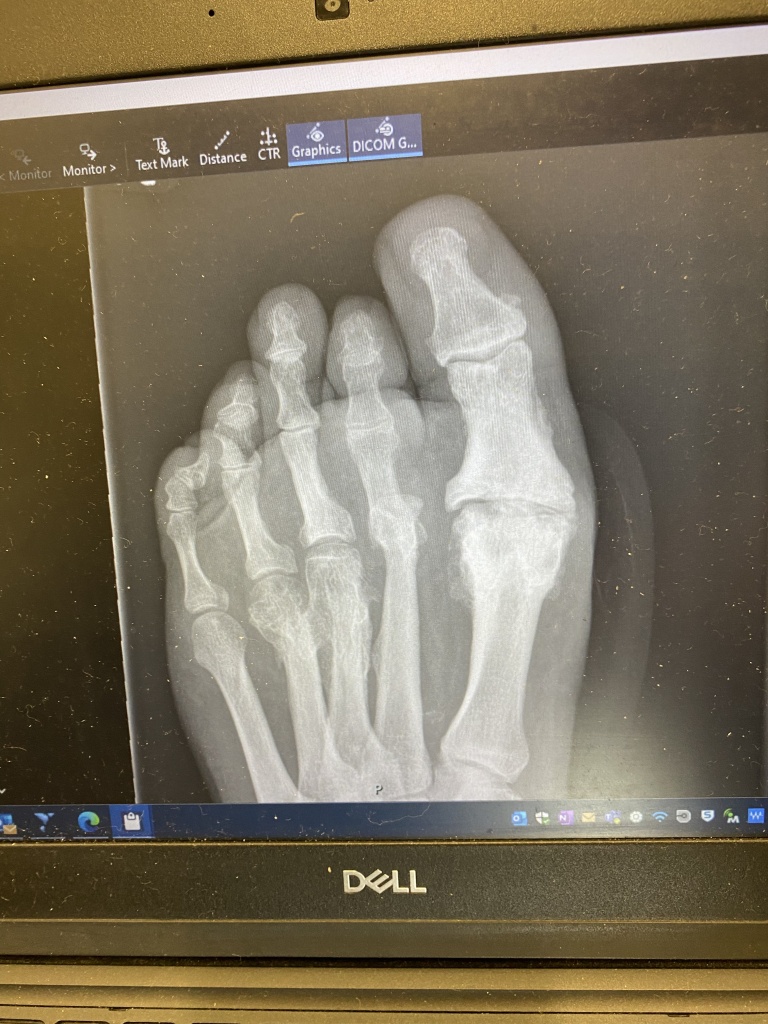
The picture above shows the issue.
Second toe from the right (next to the “Big Toe”) is dislocated 2nd joint and the bones are pointing down (hence the shortening of the toe) causing pressure every step I take of every single day.
Basically, I wear a hole in my foot. This is the third time it happened. There very likely be a 4th, 5th, 6th……. Who knows?
The story of my first two ulcers is well documented along with the gory pics.
This one won’t be.
Once the first two ulcers had healed, I reflected and realised that I had burned out due to the almost 2 years of treatment and that had taken several months to manifest and lasted the rest of the treatment.
Today I realised that I was already burned out with ulcer number 3 and the prospect of months of treatment and the certainty (in my head) that this will keep happening and there is no end game.
Breaking down in tears literally begging my podiatrist for surgery to remove the dislocated bones was not the subtlest of indications of my burn out I know.
At EASD leas week I attended a workshop about the FDA Rescue research on self-harm and suicide in people living with diabetes. I have not seen the data but I wonder if and how much diabetes related complications factor in these cases.
Please, please, please continue to #TalkAboutComplications
Grumps.